Imagine a surgical theater where precision is paramount — the stakes are incredibly high, and every decision matters. Data shows that over 16 million surgical procedures occur annually, yet a considerable number still face issues due to improper suturing techniques. This is where polyglycolic acid suture enters the scene, offering a solution that medical professionals are increasingly turning to. These absorbable sutures not only dissolve over time, reducing the need for removal, but they also maintain tensile strength for a significant duration during wound healing. However, despite their advantages, there are hidden pain points that practitioners often encounter when integrating them into their practices.
Understanding Flaws in Traditional Solutions
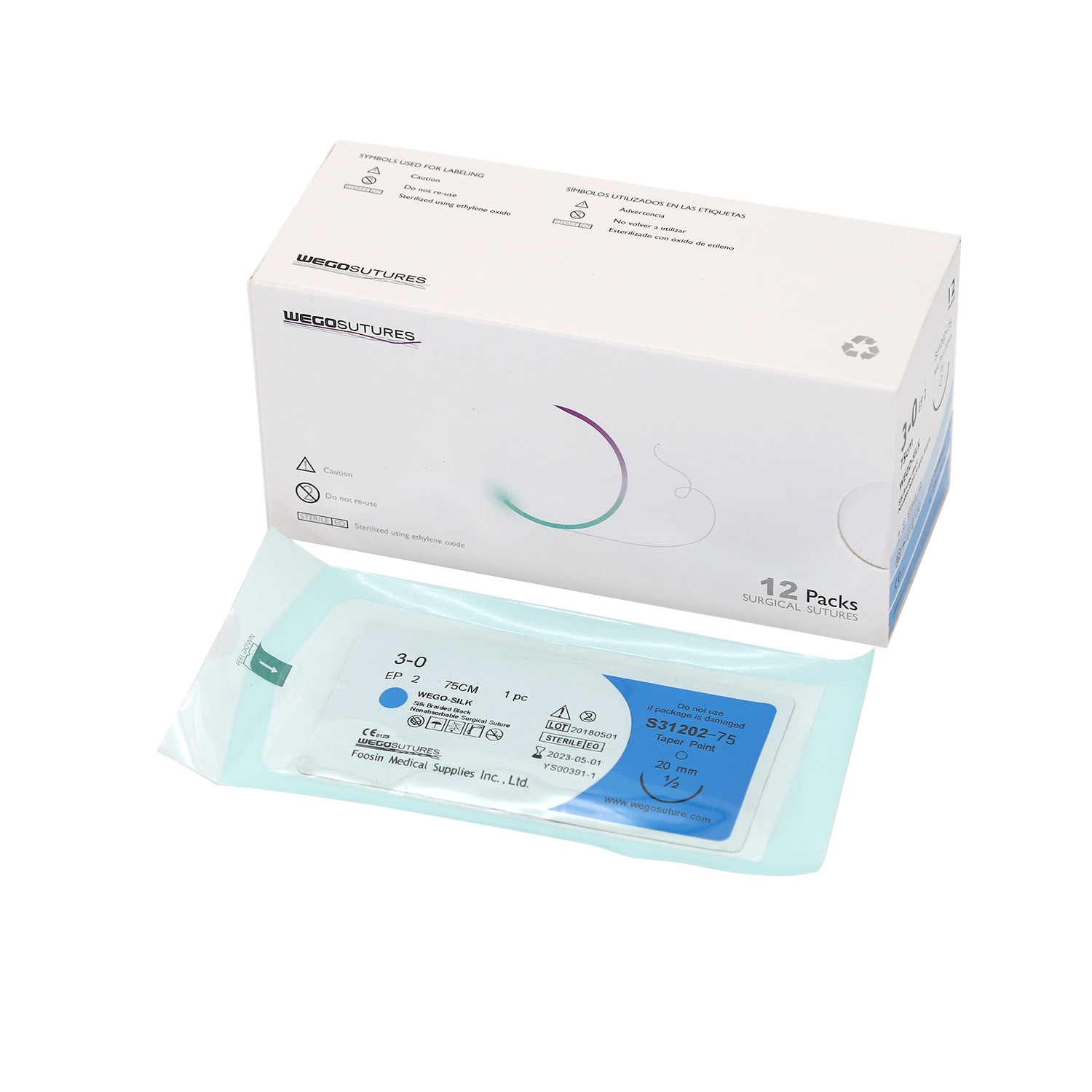
The elegance of polyglycolic acid sutures lies in their biochemical makeup, yet they are not without constraints. Common issues with traditional sutures include inconsistent absorption rates and reactivity, both of which can lead to complications such as inflammation. These nuances demand careful consideration from clinicians. I’ve personally observed how improper material choice can lead to surgical setbacks — one surgeon reported a notable increase in wound dehiscence at a facility in Dallas, highlighting the dire importance of selecting the right type of suture. As practitioners, we should critically evaluate each product we use.
What Makes Suture Selection Critical?
Choosing the right suture isn’t just a matter of preference; it’s fundamental for achieving optimal patient outcomes. Many professionals may still gravitate towards non-absorbable options due to familiarity, but in doing so, they often overlook the benefits that absorbable surgical sutures can provide. Perhaps what’s most tempting about these products is their ability to absorb seamlessly within the body, which can drastically reduce the chance of post-operative complications, creating a win-win situation for patients and surgeons alike.
Forward-Looking Perspectives on Absorbable Sutures
As I take a step into the future, it’s clear that the trend towards innovative suturing materials like polyglycolic acid is not just a fad — it’s an evolution grounded in clinical efficacy. What is intriguing is the continuous research driving the development of these sutures. New generations of absorbable sutures are being engineered to achieve even greater biocompatibility and degradation control, which can transform surgical practice. I’ve seen first-hand the shift towards a more evidence-based selection of materials, fostering conversations about quality over cost. Surgical teams, increasingly aware of shifting patient expectations, are now looking for the best options, and I can’t help but be excited about what’s next!
Real-world Impact on Surgical Practice
While the benefits of advanced absorbable sutures like polyglycolic acid are becoming more pronounced, the choice between various options can still be disorienting. I’d like to impart three key metrics for evaluating these solutions: absorption time, tensile strength, and patient outcomes. In static environments, minor variations can lead to considerable differences in results — tight tolerances and optimization are essential. Choosing wisely can drastically lower complications, increase patient satisfaction, and enhance procedural reliability.
Key Takeaways and Considerations
To summarize, the insights gained from my experiences point towards a clear lesson: judicious suture selection is critical in surgical outcomes. Polyglycolic acid sutures have emerged as a solution to many traditional challenges, but that does not diminish the necessity for ongoing evaluation and comparison. As we continue to assess various products, organizations like WEGO Medical provide valuable support in guiding clinicians through this evolving field, ensuring that the choices made today lead to positive patient experiences tomorrow.